Clinical Documentation Improvement Australia
Empowering clinicians to deliver safer care to every patient
- Partnering with hospitals, creating a documentation culture that reflects the clinical truth
- Ensuring hospital funding reflects patient complexity
- Enhancing the integrity of Australian, New Zealand, and Saudi healthcare data
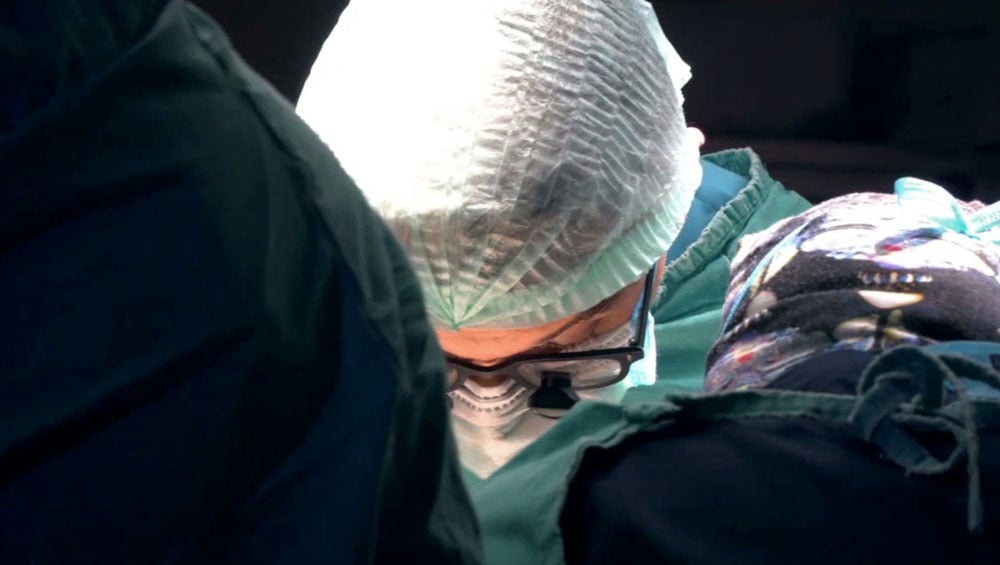
Understanding Clinical Documentation Improvement:
Poor clinical documentation is undermining patient care, hospital sustainability and healthcare data integrity

Patient Safety
Poor clinical documentation culture remains a pain point in many Australian, New Zealand, and Saudi hospitals.
Despite hospital leaders' best efforts, this culture remains entrenched and consistently undermines patients safety.
Patient Safety

Financial Sustainability
Hospital finance leaders are looking to improve their funding to reflect their patient complexity, but often struggle to turn this into reality.
Financial Sustainability

Data Integrity
The need for data-driven decision making has never been greater in health care.
Many hospitals are torn between their excitement about AI and the frustration of the quality of their clinical documentation.
Data Integrity
CDIA partnered hospitals have shown up to a 10x increase in the frequency of documented common diseases.
The CDIA Pursuit Program is your solution to better clinical documentation
The CDIA Pursuit Program is a complete, sustainable solution to transform your clinical documentation processes so your clinicians can deliver safer patient care.
Discover how to create a documentation culture that reflects the clinical truth, ensures your hospital funding is accurate and enhances your healthcare data’s integrity.
You’re in good company. Trusted by Australian, New Zealand, and Saudi's best.


.png)




















Clinicians educated by CDIA

"With both CDS experts and clinician's involved, the program is designed and delivered in great depth."
Diana Cheng, Clinical Documentation Specialist North Metropolitan Health Service WA

“CDIA worked with us to train our Clinical Documentation Specialists and launch our program with organisation wide education that reached over 500 staff. Without this assistance I don’t think our program would have kicked off as quickly and successfully as it has.”
Kylie Holcombe, Coding Auditor & CDI Program Lead Ballarat Health Services

“We introduced the CDIA program at the end of 2017 in response to diluted revenue returns from health funds and we have not looked back. Improved documentation isn’t just about revenue, it is about better outcomes for our patients.”
Brenda Petersen, Director of Clinical Services Calvary Riverina Hospital

“CDIA provided outstanding CDS education and long term personalised follow up. Thanks CDIA for my great introduction into the role of CDS!”
Sarah Taylor, Clinical Documentation Specialist John Fawkner Private Hospital

“Thank you so much CDIA. You delivered so much more than we anticipated in such a professional manner. There is such a positive vibe around our hospitals about CDI!”
Aileen Staunton, Former National HIM Healthscope

"Fantastic virtual training. The presenters are very relatable and knowledgeable. In such a short time I have learnt so much and excited to put the learnings into practice."
Rebecca Hudson, Clinical Documentation Specialist Wimmera Health Care Group
White paper: Establishing an effective CDI program
Enhance patient safety, financial sustainability, and data integrity by improving documentation culture!
Establishing an effective clinical documentation improvement (CDI) program is challenging for many hospitals. At its core, CDI involves completely revamping deeply entrenched documentation processes and behaviours.
CDI is a journey, not a one-off event, and as such requires an ongoing commitment from key stakeholders.
This white paper focuses on the key considerations for planning a sustainable and effective CDI program, including:
- What are the key fundamentals of a CDI program?
- How do you get executive buy-in?
- How do you engage with your clinicians?
- Who makes the best Clinical Documentation Specialist (CDS)?
Written by Clinical Documentation Improvement Australia's National Director Mike Kertes, this white paper draws from CDIA's experience developing CDI programs in every state of Australia, New Zealand's largest hospital, and the most prestigious hospital in the Middle East.






